Testing Diabetes Melitus Patients Over 40 For Peripheral Arterial Disease (PAD)
Friday, September 01, 2023
by Jay Long, MD
The developed world continues to be ravaged by complications of diabetes mellitus, ischemic heart disease, and strokes. These entities overlap in their contributions to being the leading causes of morbidity and mortality, and the incidence of these diseases continues to rise.
The health care industry made cancer screening a priority of early detection to reduce mortality and enable less invasive and less costly treatment modalities to be more effective. A similar approach of combined efforts is needed to improve outcome for patients with diabetes mellitus and underlying atherosclerotic disease.
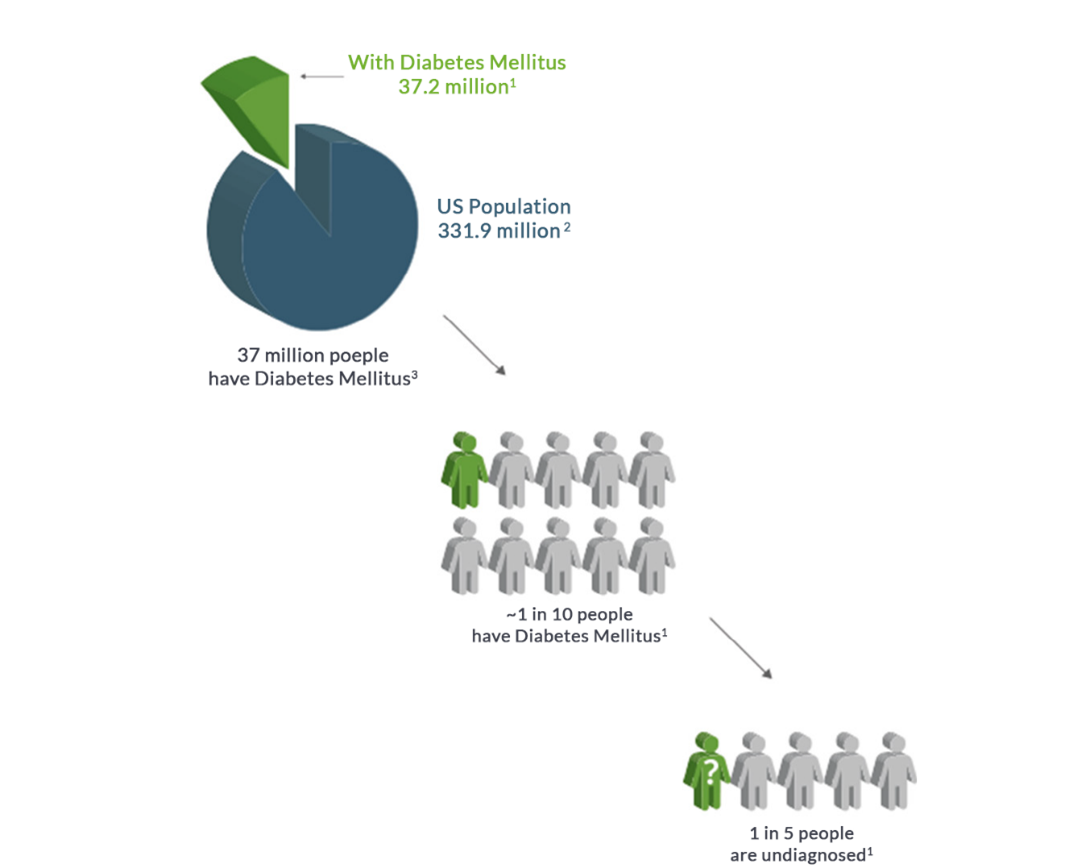
1 in 10 Americans have Diabetes Mellitus1
- Total: 37.2 million people have diabetes (11.3% of the US population)1-2
- Diagnosed: 28.7 million people, including 28.5 million adults1
- Undiagnosed: 8.5 million people (23.0% of adults)1
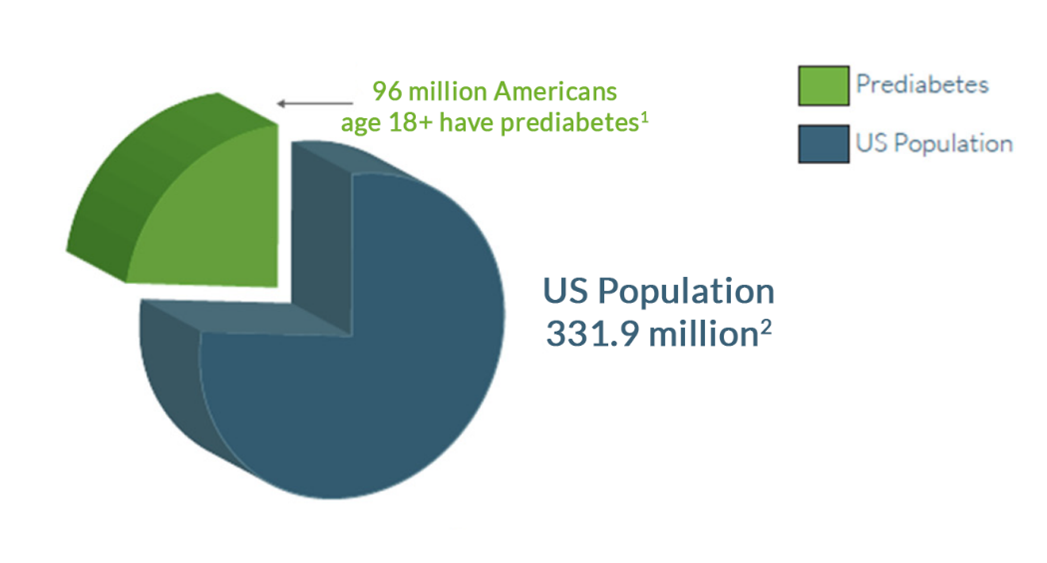
1 in 3 Americans Have Prediabetes Mellitus1
- Patients 65 years or older: 26.4 million people aged 65 years or older (48.8%) have prediabetes9
Diabetes Mellitus (DM) and Peripheral Arterial Disease (PAD)
The strong correlation between DM and PAD points to the need for an effective screening program to identify those patients most likely to benefit from early recognition and risk factor modification programs.
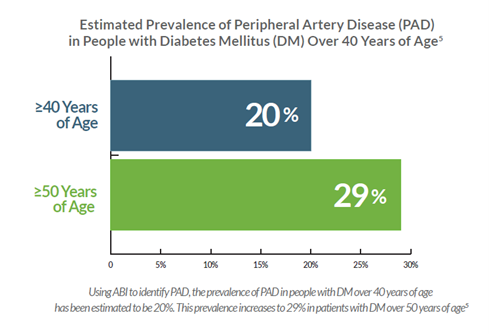
These metrics were derived using a cuff-based ABI pressure test to detect PAD.5 However, DM patients commonly present with non-compressible arteries due to advanced calcified atherosclerotic plaque which can lead to a false negative test when using pressure-based technologies. This means the true incidence rate of PAD is likely much higher.
Community outreach healthcare strategies are being deployed to measure A1C, cholesterol, and lipids, in addition to BP and weight. These screening programs have also been paired with early detection of cancer. What is lacking is a coordinated effort to detect early PAD as a marker for the atherosclerotic diathesis.
Atherosclerosis is a systemic disease; its detection anywhere is a predictor for adverse cardiovascular outcomes. Historically, diagnostic modalities using techniques like ABI have been limited to outpatient facilities simply due to the bulky nature of the equipment. Limited access to testing coupled with the lack of accuracy of ABI in patients reduces the opportunity for early detection in this PAD population.
Two studies recently published in the Journal of Vascular Surgery (JVS) and American Journal of Preventive Medicine (AJPM) documented that a positive PAD test in patients without a prior diagnosis of PAD was an independent outcomes indicator of all-cause mortality and major adverse cardiovascular events.10-11 These studies were performed using QuantaFlo® PAD – a fast, portable, FDA-cleared device which aids in the early detection of peripheral arterial disease. With this device it was possible to conduct these screening exams in either the outpatient community or home setting.
QuantaFlo PAD uses infrared sensor technology and a proprietary algorithm to measure arterial flow volumes as it is more sensitive than other pressure-based modalities, especially in the presence of calcified atherosclerotic plaque, thus simplifying the detection of early pre-clinical disease.
To optimize healthcare performance, the Institute for Healthcare Improvement developed the Triple Aim Initiative.8 This initiative is composed of three dimensions which are: better care for individuals, better health for populations and lower per capita costs. The first metric which is centered on improving the patient’s experience is a place where QuantaFlo PAD testing can easily be incorporated into routine clinic or home-based screening for pre-diabetes and ongoing management of patients with diabetes. The results are immediately available to the provider, who can implement risk-factor modification.
Offering an effective screening program to detect the presence of PAD in diabetic patients over 40 years of age combined with risk factor reduction programs, will be an important modality to address the leading causes of morbidity, mortality, and costs in the US and throughout the developed world.
Conclusion
In every disease entity, a successful outcome is the direct result of early detection and risk factor modifications. Historically, DM and PAD efforts have focused primarily on those patients already suffering from the complications of DM or with a major atherosclerotic burden. These patients are inherently more expensive to manage, have worse clinical outcomes, and are less likely to have value from their therapeutic interventions.
Early detection of both DM and PAD in the pre-clinical state may reduce the costs of care and reduce long-term complications of DM and all the sequelae of atherosclerosis, such as ischemic heart disease, stroke, renal failure, and amputation.
References
- DIABETES IN THE U.S A. SNAPSHOT DIABETES 37 million people have diabetes PREDIABETES. (n.d.). https://www.cdc.gov/diabetes/images/library/socialmedia/DiabetesInTheUS_Print.pdf
- 2022 State of the Union: US Population. (n.d.). USAFacts. Retrieved June 7, 2023, from https://usafacts.org/state-of-the-union-2022/population/
- Xu, J., Murphy, S., Kochanek, K., & Arias, E. (2022). Mortality in the United States, 2021 Key findings Data from the National Vital Statistics System. https://www.cdc.gov/nchs/data/databriefs/db456.pdf
- (2021, December 21). Prediabetes - Your Chance to Prevent Type 2 Diabetes. Centers for Disease Control and Prevention. https://www.cdc.gov/diabetes/basics/prediabetes.html
- Thiruvoipati, T., Kielhorn, C. E., & Armstrong, E. J. (2015). Peripheral artery disease in patients with diabetes: Epidemiology, mechanisms, and outcomes. World journal of diabetes, 6(7), 961–969. https://doi.org/10.4239/wjd.v6.i7.961
- AHA: One in three black Americans will experience PAD. (n.d.). Www.mdedge.com. Retrieved June 7, 2023, from https://www.mdedge.com/cardiology/article/104904/peripheral-vascular-disorders/aha-one-three-black-americans-will
- Centers for Disease Control and Prevention. (2022, December 30). Prediabetes - your chance to prevent type 2 diabetes. Centers for Disease Control and Prevention. https://www.cdc.gov/diabetes/basics/prediabetes.html
- The IHI triple aim: IHI. Institute for Healthcare Improvement. (n.d.). https://www.ihi.org/Engage/Initiatives/TripleAim/Pages/default.aspx
- Centers for Disease Control and Prevention. (2022a, June 29). National Diabetes Statistics Report. Centers for Disease Control and Prevention. https://www.cdc.gov/diabetes/data/statistics-report/index.html
- Smolderen, K. G., Heath, K., Scherr, T., Bauzon, S. R., Howell, A. N., & Mena-Hurtado, C. (2022). The Nevada peripheral artery disease screening effort in a Medicare Advantage population and subsequent mortality and major adverse cardiovascular event risk. Journal of vascular surgery, 75(6), 2054–2064.e3. https://doi.org/10.1016/j.jvs.2022.01.134
- Howell, S. C., & Master, R. C. (2023, February 27). Clinical evaluation of volume plethysmography as an aid for diagnosis of heart failure in the Primary Care Setting. Journal of Preventive Medicine. https://preventive-medicine.imedpub.com/clinical-evaluation-of-volume-plethysmography-as-an-aid-for-diagnosis-of-heart-failure-in-the-primary-care-setting.php?aid=50066
About the Author
Dr. Long is a retired Board-Certified Vascular Surgeon. Dr. Long's areas of expertise are noninvasive diagnosis of vascular and venous insufficiency and management of venous diseases. He specialized in open arterial reconstructive procedures and was one of the first in Northern California to move towards minimally invasive reconstructive venous procedures.
